Achilles tendinopathy is a more appropriate term for inflammation of the Achilles tendon, compared to Achilles tendonitis. This condition signifies that the tendon is weakened and not functioning properly, making it susceptible to small injuries from continuous usage.
Key Takeaway
- A preferable term over Achilles tendonitis, indicates a weakened and dysfunctioning tendon prone to microinjuries from overuse.
- Strategies include avoiding aggravating activities, using pain relief medications and ice, wearing supportive footwear, employing massage or foam rolling, and kinesiology tape application, along with specific eccentric exercises.
- When non-surgical methods fail, surgical interventions like tendon repair, debridement, tendon transfer, or gastrocnemius recession may be considered, followed by physical therapy for recovery.
- Characterized by pain and swelling in the tendon at the lower leg’s back, it occurs due to repetitive stress, with two types: non-insertional (middle tendon damage) and insertional (heel bone attachment).
- Diagnosis involves physical exams and imaging tests like X-rays, MRIs, or ultrasound. The RICE protocol (Rest, Ice, Compression, Elevation) serves as an effective home remedy.
Pain Relief and Exercise Modification
For relief and management of pain and challenges encountered during running or daily activities, consider these suggestions. It’s important to seek advice from a healthcare professional before starting any medical interventions, and avoid self-treatment without proper guidance.
Exercise Adjustment and Relative Rest

Initially, steer clear of activities like hill running or walking that might exacerbate the Achilles issue. Tailoring your training regimen and specific exercises is crucial.
Alleviating Pain
Over-the-counter anti-inflammatory medications, such as ibuprofen and acetaminophen, along with topical gels, can be effective in managing pain. This can help maintain your running and training routines. Applying ice for 10-15 minutes multiple times a day can also be beneficial. However, consult your doctor before taking any medication.
Proper Footwear
Opt for supportive, cushioned shoes. Consider using a heel lift inside your shoe to increase plantarflexion, which can reduce the load on the Achilles tendon.
Massage and Foam Rolling Techniques

Start from the lower leg and work up to the calf. This helps relax the muscle, easing tension on the Achilles tendon. Deep friction massage and tendon mobilization can enhance tissue elasticity.
Using Kinesiology Tape

Applying this tape to the calf and Achilles can alleviate tension. It stabilizes the injury by adhering lightly to the skin and compressing the surrounding tissues, allowing for synchronized movement with the body.
Eccentric Strengthening Exercises
Early-stage Achilles tendonitis may benefit from these exercises. They help stiffen and lengthen the myotendinous unit, reducing neovascularization in the tendon. A regimen of straight leg and bent-knee heel drops, performed in three sets of 15 reps twice daily for 12 weeks, can be effective. As pain decreases, gradually increase the load.
Advanced Treatment Options
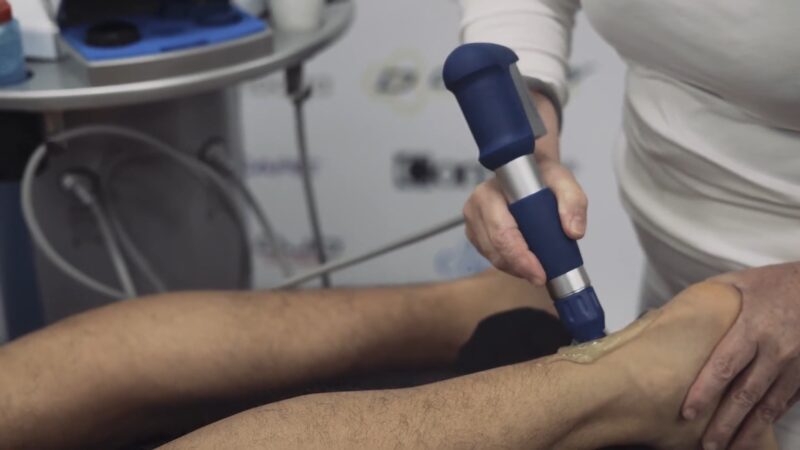
If available, consider these treatments:
- Therapeutic Ultrasound: This can diminish swelling in soft tissue disorders’ acute inflammatory stages, relieve pain, and improve functionality, while also promoting collagen production.
- Extracorporeal Shockwave Therapy (ESWT): ESWT helps initiate tendon regeneration and has shown efficacy in treating chronic Achilles tendonitis, though optimal doses and durations are yet to be determined.
- Corticosteroid Injections: These can reduce pain and inflammation but may have adverse effects and weaken the tendon.
- Platelet-Rich Plasma (PRP) Therapy: PRP injections at the injury site can accelerate healing and are known to increase types I and III collagen
Surgical Interventions for Achilles Tendinopathy
In cases where six months of non-operative treatments don’t yield improvement, surgical repair of the Achilles tendon might be necessary. The surgical approach depends on the damage’s extent and location, along with other factors like the severity of the tendinopathy.
Surgical Techniques:
- Repairing a Completely Ruptured Tendon: This involves an incision in the lower leg’s back and suturing the torn tendon. If the tear is severe, reinforcement with other tendons may be needed.
- Removing Thickened Tissue: For Achilles tendonitis, surgery might involve excising fibrous tissue from the healthy tendon.
- Post-Surgery Rehabilitation: Physical therapy is often required to strengthen the tendon and leg muscles.
Specific Surgical Procedures:
- Debridement and Repair: Applied when less than half of the tendon is damaged, it involves removing the damaged part and suturing the remainder. Bone spurs removal may occur concurrently, depending on the tendonitis type.
- Debridement with Tendon Transfer: Used when over half of the tendon is damaged, it strengthens the damaged tendon by transferring the tendon that assists in pointing the big toe downward to the heel bone. Return to competitive sports or running may not be possible for some, depending on the damage extent.
- Gastrocnemius Recession: This lengthens one of the calf muscles to reduce strain on the Achilles tendon, helping those who have difficulty flexing their feet despite regular muscle stretching.
Possible Surgical Complications:
- Infection, slow wound healing, nerve and soft tissue damage, and bleeding are rare but possible complications.
Innovative Treatments:
- Therapeutic Laser Therapy: This non-invasive method uses light energy to stimulate cell activity, enhancing circulation, reducing inflammation, swelling, muscle spasms, stiffness, and pain. It’s a drug-free and surgery-free option, often complementing traditional physical therapy for Achilles tendonitis.
Most patients experience positive outcomes from surgery, with recovery typically taking about a year. The more extensive the tendon involvement, the longer the recovery and the lower the likelihood of returning to sports. Post-surgical physical therapy is essential for a full recovery.
What is Achilles tendonitis?
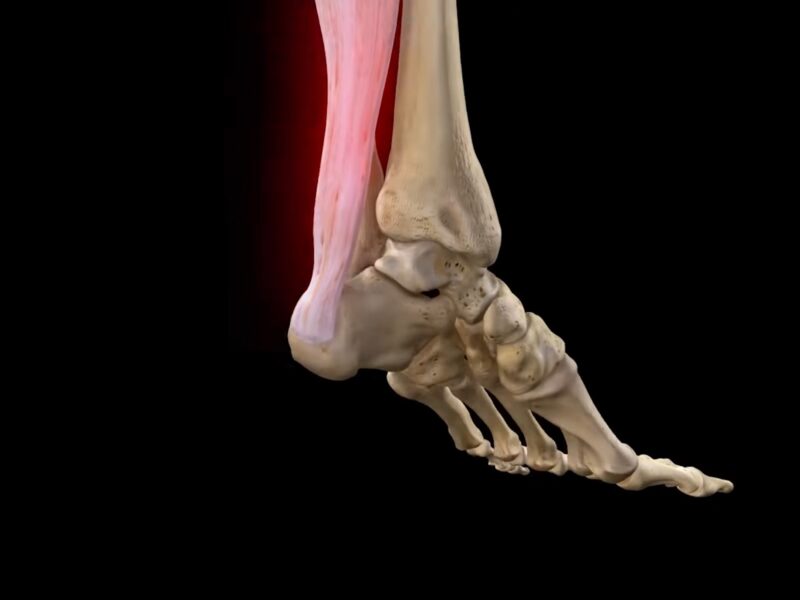
Achilles tendonitis is a widespread ailment where the large tendon at the back of your lower leg becomes swollen and sore.
This tendon, while robust and capable of enduring the stress from activities like running and jumping, is prone to tendonitis. This condition stems from wear and tear and excessive use.
There are two varieties of Achilles tendonitis:
- Non-insertional Achilles Tendonitis: In this type, the fibers in the tendon’s middle section start to break down, leading to swelling and thickening of the tendon. It’s more frequently seen in younger, active individuals.
- Insertional Achilles Tendonitis: This occurs where the tendon connects to the heel bone, at the lower part of the heel. It can affect anyone, regardless of their physical activity levels. Often, those with insertional Achilles tendonitis also develop bone spurs.
What are the symptoms of Achilles tendonitis?
- Experiencing pain at the back of the heel during activities like walking or running.
- The presence of bruising, redness, or swelling around the inflamed area.
- A tender Achilles tendon in the morning, particularly when first placing weight on your feet after waking.
- Stiffness or difficulty in moving the foot or ankle.
- Increased pain during and after engaging in high-intensity activities such as running or jumping.
- Discomfort in the area where the tendon connects to the heel bone.
- Recurring pain following a period of rest or inactivity.
- Often, there is initial pain, soreness, or stiffness in the morning, or after prolonged periods of sitting or lying down.
- Over time, a tender, painful lump may develop on the tendon.
Causes

Achilles tendonitis typically arises from repeated strain on the tendon, not from a single incident. This often occurs when individuals push their bodies excessively hard or too quickly.
Contributing factors to this condition include:
- Leg Length Discrepancy: Differences in leg length can contribute to tendonitis.
- Overuse: Continuous or excessive use of the Achilles tendon.
- Rapid Intensity Increase: Quickly amplifying the intensity of physical activity.
- Sudden Training Surface Changes: Switching abruptly from soft to hard training surfaces.
- Inappropriate Footwear: Shoes that do not provide adequate support or fit.
- Muscle Tightness or Fatigue: Muscles that are too tight or overworked.
- Insufficient Stretching: Not stretching adequately before engaging in physical activities.
- Foot Alignment Issues: An unstable or deviated axis of the rear foot.
Risk factors enhancing the likelihood of developing Achilles tendonitis:
- Obesity
- Age
- Diabetes
- Inadequate Warm-Up: Not warming up properly before exercising.
- Ill-Fitting Running Shoes: Wearing poorly fitting shoes while running.
- Uneven or Uphill Running Surfaces
- Sudden Speed Changes
- Participation in Certain Sports: Like football, baseball, volleyball, and tennis.
- Certain Medications: Such as glucocorticoids and fluoroquinolones.
Immediate treatment and reduced pressure on the lower limbs are recommended upon noticing signs of Achilles tendonitis to prevent further deterioration.
Diagnosing
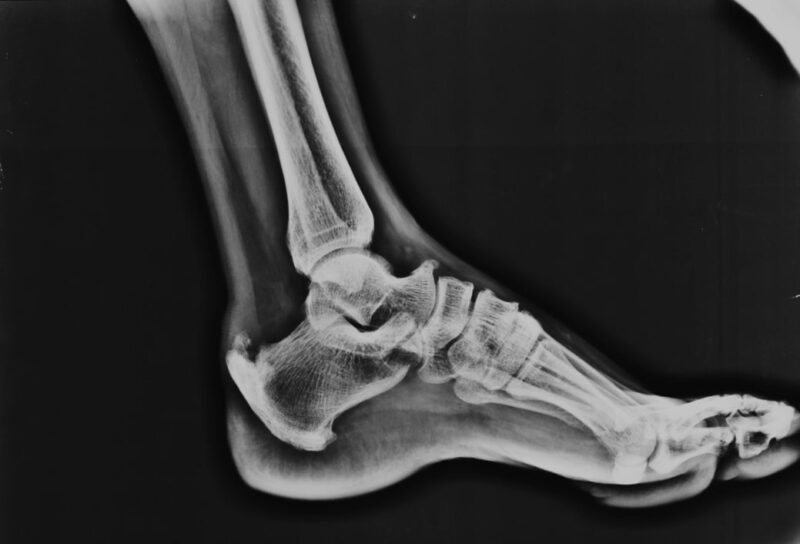
Your doctor will use the following methods to diagnose Achilles tendonitis:
- Physical Examination: Examining your calf, heel, foot, and ankle for symptoms, palpating the affected area to locate pain or discomfort, and inquiring about the injury’s history.
- Imaging Tests: These may include:
- X-rays: For visualizing leg bones and foot, checking for bone calcification.
- Magnetic Resonance Imaging (MRI) Scans: To identify tendon ruptures or tissue degeneration.
- Ultrasound: To assess tendon damage or inflammation.
As a home remedy, the RICE protocol (Rest, Ice, Compression, and Elevation) is often recommended and can be effective in treating Achilles tendonitis.
FAQ
Can diet affect Achilles tendonitis recovery?
Yes, a balanced diet rich in anti-inflammatory foods and essential nutrients can aid in reducing inflammation and promoting tendon healing.
Are there any specific stretches recommended for Achilles tendonitis?
Gentle calf stretches and Achilles tendon stretches can help improve flexibility and reduce tension in the tendon.
Is it advisable to use orthotic inserts for Achilles tendonitis?
Custom orthotic inserts can provide additional heel and arch support, helping to alleviate strain on the Achilles tendon.
How can I prevent Achilles tendonitis in the future?
Regular stretching, proper footwear, gradual training intensity increases, and avoiding overuse can help prevent recurrence.
Is acupuncture effective for treating Achilles tendonitis?
Some individuals find relief from Achilles tendonitis symptoms through acupuncture, but it’s essential to consult with a healthcare professional first.
Can yoga help in recovering from Achilles tendonitis?
Yoga, particularly poses that focus on lower leg flexibility and strength, can be beneficial in the recovery process.
Are there any natural remedies recommended for Achilles tendonitis?
Natural remedies like turmeric, ginger, and omega-3 fatty acids may help reduce inflammation, but they should be used in conjunction with other treatments.
Conclusion
Achilles tendonitis, while a common and sometimes stubborn condition, can be effectively managed and healed with the right combination of rest, therapy, and lifestyle adjustments.
